X-ray
From Wikipedia, the free encyclopedia
This article is about the form of radiation. For the method of imaging, seeRadiography. For imaging in a medical context, see Radiology. For other uses, see X-ray (disambiguation).
X-radiation (composed of X-rays) is a form ofelectromagnetic radiation. X-rays have awavelength in the range of 0.01 to 10nanometers, corresponding tofrequencies in the range 30 petahertz to 30exahertz (3 × 1016 Hz to 3 × 1019 Hz) and energies in the range 120eV to 120 keV. They are shorter in wavelength than UV rays and longer than gamma rays. In many languages, X-radiation is calledRöntgen radiation, afterWilhelm Conrad Röntgen, who is generally credited as their discoverer, and who had named them X-rays to signify an unknown type of radiation.[1]:1-2
X-rays from about 0.12 to 12 keV (10 to 0.10 nm wavelength) are classified as "soft" X-rays, and from about 12 to 120 keV (0.01 to 0.10 nm wavelength) as "hard" X-rays, due to their penetrating abilities.
Hard X-rays can penetrate solid objects, and their largest use is to take images of the inside of objects in diagnostic radiography and crystallography. As a result, the term X-ray is metonymically used to refer to a radiographic image produced using this method, in addition to the method itself. By contrast, soft X-rays can hardly be said to penetrate matter at all; for instance, the attenuation length of 600 eV (~ 2 nm) x-rays in water is less than 1 micrometer.[4] X-rays are a form of ionizing radiation, and exposure to them can be a health hazard.
The distinction between X-rays and gamma rays has changed in recent decades. Originally, the electromagnetic radiation emitted by X-ray tubes had a longer wavelength than the radiation emitted by radioactive nuclei (gamma rays).[2] Older literature distinguished between X- and gamma radiation on the basis of wavelength, with radiation shorter than some arbitrary wavelength, such as 10−11 m, defined as gamma rays.[3] However, as shorter wavelength continuous spectrum "X-ray" sources such as linear accelerators and longer wavelength "gamma ray" emitters were discovered, the wavelength bands largely overlapped. The two types of radiation are now usually distinguished by their origin: X-rays are emitted by electrons outside the nucleus, while gamma rays are emitted by the nucleus.[2][4][5][6]
Contents[hide] |
[edit]Units of measure and exposure
The measure of X-rays ionizing ability is called the exposure:
- The coulomb per kilogram (C/kg) is the SI unit of ionizing radiation exposure, and it is the amount of radiation required to create one coulomb of charge of each polarity in one kilogram of matter.
- The roentgen (R) is an obsolete traditional unit of exposure, which represented the amount of radiation required to create one electrostatic unitof charge of each polarity in one cubic centimeter of dry air. 1.00 roentgen = 2.58×10−4 C/kg
However, the effect of ionizing radiation on matter (especially living tissue) is more closely related to the amount of energy deposited into them rather than thecharge generated. This measure of energy absorbed is called the absorbed dose:
- The gray (Gy), which has units of (Joules/kilogram), is the SI unit of absorbed dose, and it is the amount of radiation required to deposit one joule of energy in one kilogram of any kind of matter.
- The rad is the (obsolete) corresponding traditional unit, equal to 10 millijoules of energy deposited per kilogram. 100 rad = 1.00 gray.
The equivalent dose is the measure of the biological effect of radiation on human tissue. For X-rays it is equal to the absorbed dose.
- The sievert (Sv) is the SI unit of equivalent dose, which for X-rays is numerically equal to the gray (Gy).
- The Roentgen equivalent man (rem) is the traditional unit of equivalent dose. For X-rays it is equal to the rad or 10 millijoules of energy deposited per kilogram. 1.00 Sv = 100 rem.
Medical X-rays are a significant source of manmade radiation exposure, accounting for 58% in the United States in 1987, but since most radiation exposure is natural (82%), medical X-rays only account for 10% of totalAmerican radiation exposure.[7]
Reported dosage due to dental X-rays seems to vary significantly. Depending on the source, a typical dental X-ray of a human results in an exposure of perhaps, 3,[8] 40,[9] 300,[10] or as many as 900[11] mrems (30 to 9,000 μSv).
[edit]Medical physics
| Target | Kβ₁ | Kβ₂ | Kα₁ | Kα₂ |
|---|---|---|---|---|
| Fe | 0.17566 | 0.17442 | 0.193604 | 0.193998 |
| Co | 0.162079 | 0.160891 | 0.178897 | 0.179285 |
| Ni | 0.15001 | 0.14886 | 0.165791 | 0.166175 |
| Cu | 0.139222 | 0.138109 | 0.154056 | 0.154439 |
| Zr | 0.070173 | 0.068993 | 0.078593 | 0.079015 |
| Mo | 0.063229 | 0.062099 | 0.070930 | 0.071359 |
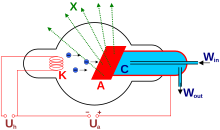
X-rays are generated by anX-ray tube, a vacuum tubethat uses a high voltage to accelerate the electronsreleased by a hot cathodeto a high velocity. The high velocity electrons collide with a metal target, theanode, creating the X-rays.[15] In medical X-ray tubes the target is usuallytungsten or a more crack-resistant alloy of rhenium(5%) and tungsten (95%), but sometimes molybdenum for more specialized applications, such as when soft X-rays are needed as in mammography. In crystallography, acopper target is most common, withcobalt often being used when fluorescence from iron content in the sample might otherwise present a problem.
The maximum energy of the produced X-ray photon is limited by the energy of the incident electron, which is equal to the voltage on the tube, so an 80 kV tube cannot create X-rays with an energy greater than 80 keV. When the electrons hit the target, X-rays are created by two different atomic processes:
- X-ray fluorescence: If the electron has enough energy it can knock an orbital electron out of the inner electron shell of a metal atom, and as a result electrons from higher energy levels then fill up the vacancy and X-ray photons are emitted. This process produces an emission spectrum of X-ray frequencies, sometimes referred to as the spectral lines. The spectral lines generated depend on the target (anode) element used and thus are called characteristic lines. Usually these are transitions from upper shells into K shell (called K lines), into L shell (called L lines) and so on.
- Bremsstrahlung: This is radiation given off by the electrons as they are scattered by the strong electric field near the high-Z (proton number) nuclei. These X-rays have a continuous spectrum. The intensity of the X-rays increases linearly with decreasing frequency, from zero at the energy of the incident electrons, the voltage on the X-ray tube.
So the resulting output of a tube consists of a continuous bremsstrahlung spectrum falling off to zero at the tube voltage, plus several spikes at the characteristic lines. The voltages used in diagnostic X-ray tubes, and thus the highest energies of the X-rays, range from roughly 20 to 150 kV.[16]
In medical diagnostic applications, the low energy (soft) X-rays are unwanted, since they are totally absorbed by the body, increasing the dose. Hence, a thin metal sheet, often of aluminum, called an X-ray filter) is usually placed over the window of the X-ray tube, filtering out the low energy components in the spectrum. This is called hardening the beam.
Both of these X-ray production processes are very inefficient, with a production efficiency of only about one percent, and hence, to produce a usable flux of X-rays, a high percentage of the electric power inputted is released as waste heat. The X-ray tube must be designed to dissipate this excess heat.
Radiographs obtained using X-rays can be used to identify a wide spectrum of pathologies. Because the body structures being imaged in medical applications are large compared to the wavelength of the X-rays, the X-rays can be analyzed as particles rather than waves. (This is in contrast to X-ray crystallography, where their wave-like nature is more important because the wavelength is comparable to the sizes of the structures being imaged.)
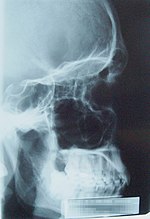
To make an X-ray image of human or animal bones, short X-ray pulses illuminate the body or limb, with radiographic film placed behind it. Any bones that are present absorb most of the X-ray photons by photoelectric processes. This is because bones have a higher electron density than soft tissues. [Note that bones contain a high percentage of calcium (20 electrons per atom), potassium (19 electrons per atom) magnesium (12 electrons per atom), and phosphorus (15 electrons per atom). The X-rays that pass through the flesh leave a latent image in the photographic film. When the film is developed, the parts of the image corresponding to higher X-ray exposure are dark, leaving a white shadow of bones on the film.
To generate an image of the cardiovascular system, including the arteries and veins (angiography) an initial image is taken of the anatomical region of interest. A second image is then taken of the same region after iodinated contrast material has been injected into the blood vessels within this area. These two images are then digitally subtracted, leaving an image of only the iodinated contrast outlining the blood vessels. The radiologist or surgeon then compares the image obtained to normal anatomical images to determine if there is any damage or blockage of the vessel.
A specialized source of X-rays which is becoming widely used in research issynchrotron radiation, which is generated by particle accelerators. Its unique features are X-ray outputs many orders of magnitude greater than those of X-ray tubes, wide X-ray spectra, excellent collimation, and linear polarization.[17]
[edit]Detectors
[edit]Photographic plate
The detection of X-rays is based on various methods. The most commonly known methods are photographic plates, photographic film in cassettes, andrare earth screens. Regardless of what is "catching" the image, they are all categorized as "Image Receptors" (IR).
Before the advent of the digital computer and before the invention of digital imaging, photographic plates were used to produce most radiographic images. The images were produced right on the glass plates. Photographic film largely replaced these plates, and it was used in X-ray laboratories to produce medical images. In more recent years, computerized and digital radiography has been replacing photographic film in medical and dental applications, though film technology remains in widespread use in industrial radiography processes (e.g. to inspect welded seams). Photographic plates are mostly things of history, and their replacement, the "intensifying screen", is also fading into history. The metal silver (formerly necessary to the radiographic & photographic industries) is a non-renewable resource. Thus it is beneficial that this is now being replaced by digital (DR) and computed (CR) technology. Where photographic films required wet processing facilities, these new technologies do not. The digital archiving of images utilizing these new technologies also saves storage space.
Since photographic plates are sensitive to X-rays, they provide a means of recording the image, but they also required much X-ray exposure (to the patient), hence intensifying screens were devised. They allow a lower dose to the patient, because the screens take the X-ray information and intensify it so that it can be recorded on film positioned next to the intensifying screen.
The part of the patient to be X-rayed is placed between the X-ray source and the image receptor to produce a shadow of the internal structure of that particular part of the body. X-rays are partially blocked ("attenuated") by dense tissues such as bone, and pass more easily through soft tissues. Areas where the X-rays strike darken when developed, causing bones to appear lighter than the surrounding soft tissue.
Contrast compounds containing barium or iodine, which are radiopaque, can be ingested in the gastrointestinal tract (barium) or injected in the artery or veins to highlight these vessels. The contrast compounds have high atomic numbered elements in them that (like bone) essentially block the X-rays and hence the once hollow organ or vessel can be more readily seen. In the pursuit of a non-toxic contrast material, many types of high atomic number elements were evaluated. For example, the first time the forefathers used contrast it was chalk, and was used on a cadaver's vessels. Unfortunately, some elements chosen proved to be harmful – for example, thorium was once used as a contrast medium (Thorotrast) – which turned out to be toxic in some cases (causing injury and occasionally death from the effects of thorium poisoning). Modern contrast material has improved, and while there is no way to determine who may have a sensitivity to the contrast, the incidence of "allergic-type reactions" are low. (The risk is comparable to that associated with penicillin.[citation needed])
[edit]Photostimulable phosphors (PSPs)
An increasingly common method is the use of photostimulated luminescence(PSL), pioneered by Fuji in the 1980s. In modern hospitals a photostimulable phosphor plate (PSP plate) is used in place of the photographic plate. After the plate is X-rayed, excited electrons in the phosphor material remain "trapped" in "colour centres" in the crystal lattice until stimulated by a laser beam passed over the plate surface. The light given off during laser stimulation is collected by a photomultiplier tube and the resulting signal is converted into a digital image by computer technology, which gives this process its common name, computed radiography (also referred to as digital radiography). The PSP plate can be reused, and existing X-ray equipment requires no modification to use them.
[edit]Geiger counter
Initially, most common detection methods were based on the ionization of gases, as in the Geiger-Müller counter: a sealed volume, usually a cylinder, with a mica, polymer or thin metal window contains a gas, a cylindrical cathode and a wire anode; a high voltage is applied between the cathode and the anode. When an X-ray photon enters the cylinder, it ionizes the gas and forms ions and electrons. Electrons accelerate toward the anode, in the process causing further ionization along their trajectory. This process, known as a Townsend avalanche, is detected as a sudden current, called a "count" or "event".
In order to gain energy spectrum information, a diffracting crystal may be used to first separate the different photons. The method is called wavelength dispersive X-ray spectroscopy (WDX or WDS). Position-sensitive detectors are often used in conjunction with dispersive elements. Other detection equipment that is inherently energy-resolving may be used, such as the aforementionedproportional counters. In either case, use of suitable pulse-processing (MCA) equipment allows digital spectra to be created for later analysis.
For many applications, counters are not sealed but are constantly fed with purified gas, thus reducing problems of contamination or gas aging. These are called "flow counters".
[edit]Scintillators
Some materials such as sodium iodide (NaI) can "convert" an X-ray photon to a visible photon; an electronic detector can be built by adding a photomultiplier. These detectors are called "scintillators", filmscreens or "scintillation counters". The main advantage of using these is that an adequate image can be obtained while subjecting the patient to a much lower dose of X-rays.
[edit]Image intensification
X-rays are also used in "real-time" procedures such asangiography or contrast studies of the hollow organs (e.g.barium enema of the small or large intestine) usingfluoroscopy acquired using an X-ray image intensifier.Angioplasty, medical interventions of the arterial system, rely heavily on X-ray-sensitive contrast to identify potentially treatable lesions.
[edit]Direct semiconductor detectors
Since the 1970s, new semiconductor detectors have been developed (silicon orgermanium doped with lithium, Si(Li) or Ge(Li)). X-ray photons are converted to electron-hole pairs in the semiconductor and are collected to detect the X-rays. When the temperature is low enough (the detector is cooled by Peltier effect or even cooler liquid nitrogen), it is possible to directly determine the X-ray energy spectrum; this method is called energy dispersive X-ray spectroscopy (EDX or EDS); it is often used in small X-ray fluorescence spectrometers. These detectors are sometimes called "solid state detectors". Detectors based oncadmium telluride (CdTe) and its alloy with zinc, cadmium zinc telluride, have an increased sensitivity, which allows lower doses of X-rays to be used.
Practical application in medical imaging started in the 1990s. Currently amorphous selenium is used in commercial large area flat panel X-ray detectors for mammography and chest radiography. Current research and development is focused around pixel detectors, such as CERN's energy resolving Medipixdetector.
Note: A standard semiconductor diode, such as a 1N4007, will produce a small amount of current when placed in an X-ray beam. A test device once used by Medical Imaging Service personnel was a small project box that contained several diodes of this type in series, which could be connected to anoscilloscope as a quick diagnostic.
Silicon drift detectors (SDDs), produced by conventional semiconductor fabrication, now provide a cost-effective and high resolving power radiation measurement. Unlike conventional X-ray detectors, such as Si(Li)s, they do not need to be cooled with liquid nitrogen.
[edit]Scintillator plus semiconductor detectors (indirect detection)
With the advent of large semiconductor array detectors it has become possible to design detector systems using a scintillator screen to convert from X-rays to visible light which is then converted to electrical signals in an array detector. Indirect Flat Panel Detectors (FPDs) are in widespread use today in medical, dental, veterinary and industrial applications.
The array technology is a variant on the amorphous silicon TFT arrays used in many flat panel displays, like the ones in computer laptops. The array consists of a sheet of glass covered with a thin layer of silicon that is in an amorphous or disordered state. At a microscopic scale, the silicon has been imprinted with millions of transistors arranged in a highly ordered array, like the grid on a sheet of graph paper. Each of these thin film transistors (TFTs) is attached to a light-absorbing photodiode making up an individual pixel (picture element). Photons striking the photodiode are converted into two carriers of electrical charge, called electron-hole pairs. Since the number of charge carriers produced will vary with the intensity of incoming light photons, an electrical pattern is created that can be swiftly converted to a voltage and then a digital signal, which is interpreted by a computer to produce a digital image. Although silicon has outstanding electronic properties, it is not a particularly good absorber of X-ray photons. For this reason, X-rays first impinge upon scintillators made from e.g. gadolinium oxysulfide or caesium iodide. The scintillator absorbs the X-rays and converts them into visible light photons that then pass onto the photodiode array.
[edit]Visibility to the human eye
While generally considered invisible to the human eye, in special circumstances X-rays can be visible.[18] Brandes, in an experiment a short time after Röntgen'slandmark 1895 paper, reported after dark adaptation and placing his eye close to an X-ray tube, seeing a faint "blue-gray" glow which seemed to originate within the eye itself.[19] Upon hearing this, Röntgen reviewed his record books and found he too had seen the effect. When placing an X-ray tube on the opposite side of a wooden door Röntgen had noted the same blue glow, seeming to emanate from the eye itself, but thought his observations to be spurious because he only saw the effect when he used one type of tube. Later he realized that the tube which had created the effect was the only one powerful enough to make the glow plainly visible and the experiment was thereafter readily repeatable. The knowledge that X-rays are actually faintly visible to the dark-adapted naked eye has largely been forgotten today; this is probably due to the desire not to repeat what would now be seen as a recklessly dangerous and potentially harmful experiment with ionizing radiation. It is not known what exact mechanism in the eye produces the visibility: it could be due to conventional detection (excitation of rhodopsin molecules in the retina), direct excitation of retinal nerve cells, or secondary detection via, for instance, X-ray induction ofphosphorescence in the eyeball with conventional retinal detection of the secondarily produced visible light.
Though X-rays are otherwise invisible it is possible to see the ionization of the air molecules if the intensity of the X-ray beam is high enough. The beamline from the wiggler at the ID11 at ESRF is one example of such high intensity.[20]
[edit]Medical uses
Since Röntgen's discovery that X-rays can identify bone structures, X-rays have been developed for their use in medical imaging, the first use was less than a month after his seminal paper on the subject.[21]Radiology is a specialized field ofmedicine. Radiologists employ radiography and other techniques for diagnostic imaging. This is probably the most common use of X-ray technology.
X-rays are especially useful in the detection of pathology of the skeletal system, but are also useful for detecting some disease processes in soft tissue. Some notable examples are the very common chest X-ray, which can be used to identify lung diseases such as pneumonia, lung cancer or pulmonary edema, and the abdominal X-ray, which can detect intestinal obstruction, free air (from visceral perforations) and free fluid (in ascites). X-rays may also be used to detect pathology such as gallstones (which are rarely radiopaque) or kidney stones which are often (but not always) visible. Traditional plain X-rays are less useful in the imaging of soft tissues such as the brain or muscle. Imaging alternatives for soft tissues are computed axial tomography (CAT or CT scanning)[22], magnetic resonance imaging (MRI) or ultrasound. The latter two do not subject the individual to ionizing radiation. In addition to plain X-rays and CT scans, physicians use fluoroscopy as an X-ray test methodology. This method often uses administration of a medical contrast material (intravenously,orally or via enema). Examples include cardiac catheterization (to examine forcoronary artery blockages) and Barium swallow (to examine for esophagealdisorders.
Since 2005, X-rays are listed as a carcinogen by the U.S. government.[23]. The use of X-rays as a treatment is known as radiotherapy and is largely used for the management (including palliation) of cancer; it requires higher radiation energies than for imaging alone.
[edit]Risks of Medical Diagnostic X-rays
X-rays are a relatively safe method of investigation and the radiation exposure is relatively low, depending upon the study. Experimental and epidemiological data, however, do not support the proposition that there is a threshold dose of radiation below which there is no increased risk of cancer.[24]Diagnostic X-rays account for 14% of the total annual radiation exposure from man-made and natural sources worldwide.[25] It is estimated that the additional radiation will increase a person's cumulative risk of getting cancer by age 75 by 0.6-1.8%.[26] The amount of absorbed radiation depends upon the type of X-ray test and the body part involved.[27] CT and fluoroscopy entail higher doses of radiation than do plain X-rays.
To place the increased risk in perspective, a plain chest X-ray or dental X-ray will expose a person to the same amount from background radiation that we are exposed to (depending upon location) everyday over 10 days.[28] Each such X-ray would add less than 1 per 1,000,000 to the lifetime cancer risk. An abdominal or chest CT would be the equivalent to 2–3 years of background radiation, increasing the lifetime cancer risk between 1 per 10,000 and 1 per 1,000.[28] These numbers are very small compared to the roughly 40% chance of developing any cancer during our lifetime.[29]
Fathers exposed to diagnostic x-rays are more likely to have infants who contract leukemia, especially if exposure is closer to conception or includes two or more X-rays of the lower gastrointestinal (GI) tract or lower abdomen.[30] The risk of radiation is greater to unborn babies, so in pregnant patients, the benefits of the investigation (X-ray) should be balanced with the potential hazards to the unborn fetus.[31][32] In the US, there are an estimated 62,000,000 CT scans performed annually, including more than 4,000,000 on children.[27] Avoiding unnecessary X-rays (especially CT scans) will reduce radiation dose and any associated cancer risk.[33]
[edit]Shielding against X-Rays
Lead is the most common shield against X-rays because of its high density (11340 kg/m3), stopping power, ease of installation and low cost. The maximum range of a high-energy photon such as an X-ray in matter is infinite; at every point in the matter traversed by the photon, there is a probability of interaction. Thus there is a very small probability of no interaction over very large distances. The shielding of photon beam is therefore exponential (with an attenuation lengthbeing close to the radiation length of the material); doubling the thickness of shielding will square the shielding effect.
The following table shows the recommended thickness of lead shielding in function of X-ray energy, from the Recommendations by the Second International Congress of Radiology.[34]
| X-Rays generated by peak voltages not exceeding | Minimum thickness of Lead |
|---|---|
| 75 kV | 1.0 mm |
| 100 kV | 1.5 mm |
| 125 kV | 2.0 mm |
| 150 kV | 2.5 mm |
| 175 kV | 3.0 mm |
| 200 kV | 4.0 mm |
| 225 kV | 5.0 mm |
| 300 kV | 9.0 mm |
| 400 kV | 15.0 mm |
| 500 kV | 22.0 mm |
| 600 kV | 34.0 mm |
| 900 kV | 51.0 mm |
[edit]Other uses
Other notable uses of X-rays include
- X-ray crystallography in which the pattern produced by the diffractionof X-rays through the closely spaced lattice of atoms in a crystal is recorded and then analysed to reveal the nature of that lattice. A related technique,fiber diffraction, was used byRosalind Franklin to discover thedouble helical structure ofDNA.[35]
- X-ray astronomy, which is an observational branch ofastronomy, which deals with the study of X-ray emission from celestial objects.
- X-ray microscopic analysis, which uses electromagnetic radiation in the soft X-ray band to produce images of very small objects.
- X-ray fluorescence, a technique in which X-rays are generated within a specimen and detected. The outgoing energy of the X-ray can be used to identify the composition of the sample.
- Industrial radiography uses X-rays for inspection of industrial parts, particularly welds.
- Paintings are often X-rayed to reveal the underdrawing and pentimenti or alterations in the course of painting, or by later restorers. Many pigmentssuch as lead white show well in X-ray photographs.
- Airport security luggage scanners use X-rays for inspecting the interior of luggage for security threats before loading on aircraft.
- Border security truck scanners use X-rays for inspecting the interior of trucks for at country borders.
- X-ray fine art photography
- Roentgen Stereophotogrammetry is used to track movement of bones based on the implantation of markers
- X-ray photoelectron spectroscopy is a chemical analysis technique relying on the photoelectric effect, usually employed in surface science.
[edit]History
[edit]Discovery
German physicist Wilhelm Röntgenis usually credited as the discoverer of X-rays because he was the first to systematically study them, though he is not the first to have observed their effects. He is also the one who gave them the name "X-rays", though many referred to these as "Röntgen rays" for several decades after their discovery.
X-rays were found emanating from Crookes tubes, experimental discharge tubesinvented around 1875, by scientists investigating the cathode rays, that is energetic electron beams, that were first created in the tubes. Crookes tubes created free electrons by ionization of the residual air in the tube by a high DCvoltage of anywhere between a few kilovolts and 100 kV. This voltage accelerated the electrons coming from the cathode to a high enough velocity that they created X-rays when they struck the anode or the glass wall of the tube. Many of the early Crookes tubes undoubtedly radiated X-rays, because early researchers noticed effects that were attributable to them, as detailed below. Wilhelm Röntgen was the first to systematically study them, in 1895.[36]
Among the important early researchers in X-rays were Ivan Pulyui, William Crookes, Johann Wilhelm Hittorf, Eugen Goldstein, Heinrich Hertz, Philipp Lenard, Hermann von Helmholtz, Nikola Tesla, Thomas Edison, Charles Glover Barkla, Max von Laue, and Wilhelm Conrad Röntgen.
[edit]Johann Hittorf
German physicist Johann Hittorf (1824–1914), a co-inventor and early researcher of the Crookes tube, found when he placed unexposed photographic plates near the tube, that some of them were flawed by shadows, though he did not investigate this effect.
[edit]Ivan Pulyui
In 1877 Ukrainian-born Pulyui, a lecturer in experimental physics at theUniversity of Vienna, constructed various designs of vacuum discharge tube to investigate their properties.[37] He continued his investigations when appointed professor at the Prague Polytechnic and in 1886 he found that sealed photographic plates became dark when exposed to the emanations from the tubes. Early in 1896, just a few weeks after Röntgen published his first X-ray photograph, Pulyui published high-quality X-ray images in journals in Paris and London.[37] Although Pulyui had studied with Röntgen at the University of Strasbourg in the years 1873–75, his biographer Gaida (1997) asserts that his subsequent research was conducted independently.[37]
[edit]Nikola Tesla
In April 1887, Nikola Tesla began to investigate X-rays using high voltages and tubes of his own design, as well as Crookes tubes. From his technical publications, it is indicated that he invented and developed a special single-electrode X-ray tube,[38][39] which differed from other X-ray tubes in having no target electrode. The principle behind Tesla's device is called theBremsstrahlung process, in which a high-energy secondary X-ray emission is produced when charged particles (such as electrons) pass through matter. By 1892, Tesla performed several such experiments, but he did not categorize the emissions as what were later called X-rays. Tesla generalized the phenomenon as radiant energy of "invisible" kinds.[40][41] Tesla stated the facts of his methods concerning various experiments in his 1897 X-ray lecture before theNew York Academy of Sciences.[42] Also in this lecture, Tesla stated the method of construction and safe operation of X-ray equipment. His X-ray experimentation by vacuum high field emissions also led him to alert the scientific community to the biological hazards associated with X-ray exposure.[43]
[edit]Fernando Sanford
X-rays were generated and detected by Fernando Sanford (1854–1948), the foundation Professor of Physics at Stanford University, in 1891. From 1886 to 1888 he had studied in the Hermann Helmholtz laboratory in Berlin, where he became familiar with the cathode rays generated in vacuum tubes when a voltage was applied across separate electrodes, as previously studied byHeinrich Hertz and Philipp Lenard. His letter of January 6, 1893 (describing his discovery as "electric photography") to The Physical Review was duly published and an article entitled Without Lens or Light, Photographs Taken With Plate and Object in Darkness appeared in the San Francisco Examiner.[44]
[edit]Philipp Lenard
Philipp Lenard, a student of Heinrich Hertz, wanted to see whether cathode rays could pass out of the Crookes tube into the air. He built a Crookes tube (later called a "Lenard tube") with a "window" in the end made of thin aluminum, facing the cathode so the cathode rays would strike it.[45] He found that something came through, that would expose photographic plates and cause fluorescence. He measured the penetrating power of these rays through various materials. It has been suggested that at least some of these "Lenard rays" were actually X-rays.[46] Hermann von Helmholtz formulated mathematical equations for X-rays. He postulated a dispersion theory before Röntgen made his discovery and announcement. It was formed on the basis of the electromagnetic theory of light.[47] However, he did not work with actual X-rays.
[edit]Wilhelm Röntgen
On November 8, 1895, German physics professor Wilhelm Röntgen stumbled on X-rays while experimenting with Lenard and Crookes tubes and began studying them. He wrote an initial report "On a new kind of ray: A preliminary communication" and on December 28, 1895 submitted it to the Würzburg's Physical-Medical Society journal.[48] This was the first paper written on X-rays. Röntgen referred to the radiation as "X", to indicate that it was an unknown type of radiation. The name stuck, although (over Röntgen's great objections) many of his colleagues suggested calling them Röntgen rays. They are still referred to as such in many languages, including German. Röntgen received the first Nobel Prize in Physics for his discovery.
There are conflicting accounts of his discovery because Röntgen had his lab notes burned after his death, but this is a likely reconstruction by his biographers:[49] Röntgen was investigating cathode rays with a fluorescentscreen painted with barium platinocyanide and a Crookes tube which he had wrapped in black cardboard so the visible light from the tube wouldn't interfere. He noticed a faint green glow from the screen, about 1 meter away. He realized some invisible rays coming from the tube were passing through the cardboard to make the screen glow. He found they could also pass through books and papers on his desk. Röntgen threw himself into investigating these unknown rays systematically. Two months after his initial discovery, he published his paper.
Röntgen discovered its medical use when he saw a picture of his wife's hand on a photographic plate formed due to X-rays. His wife's hand's photograph was the first ever photograph of a human body part using X-rays.
[edit]Thomas Edison
In 1895, Thomas Edison investigated materials' ability to fluoresce when exposed to X-rays, and found thatcalcium tungstate was the most effective substance. Around March 1896, the fluoroscope he developed became the standard for medical X-ray examinations. Nevertheless, Edison dropped X-ray research around 1903 after the death ofClarence Madison Dally, one of his glassblowers. Dally had a habit of testing X-ray tubes on his hands, and acquired a cancer in them so tenacious that both arms were amputated in a futile attempt to save his life. At the 1901 Pan-American Exposition in Buffalo, New York, an assassin shot President William McKinley twice at close range with a .32 caliber revolver. The first bullet was removed but the second remained lodged somewhere in his stomach. McKinley survived for some time and requested that Thomas Edison "rush an X-ray machine to Buffalo to find the stray bullet. It arrived but wasn't used ... McKinley died of septic shock due to bacterial infection."[50]
[edit]Frank Austin and the Frost brothers
The first medical X-ray made in the United States was obtained using a discharge tube of Pulyui's design. In January 1896, on reading of Röntgen's discovery, Frank Austin of Dartmouth College tested all of the discharge tubes in the physics laboratory and found that only the Pulyui tube produced X-rays. This was a result of Pulyui's inclusion of an oblique "target" of mica, used for holding samples of fluorescent material, within the tube. On 3 February 1896 Gilman Frost, professor of medicine at the college, and his brother Edwin Frost, professor of physics, exposed the wrist of Eddie McCarthy, whom Edwin had treated some weeks earlier for a fracture, to the X-rays and collected the resulting image of the broken bone on gelatin photographic plates obtained from Howard Langill, a local photographer also interested in Röntgen's work.[21]
[edit]The 20th century and beyond
The many applications of X-rays immediately generated enormous interest. Workshops began making specialized versions of Crookes tubes for generating X-rays, and these first generation cold cathode or Crookes X-ray tubes were used until about 1920.
Crookes tubes were unreliable. They had to contain a small quantity of gas (invariably air) as a current will not flow in such a tube if they are fully evacuated. However as time passed the X-rays caused the glass to absorb the gas, causing the tube to generate "harder" X-rays until it soon stopped operating. Larger and more frequently used tubes were provided with devices for restoring the air, known as "softeners". These often took the form of a small side tube which contained a small piece of mica: a substance that traps comparatively large quantities of air within its structure. A small electrical heater heated the mica and caused it to release a small amount of air, thus restoring the tube's efficiency. However the mica had a limited life and the restore process was consequently difficult to control.
In 1904, John Ambrose Fleming invented the thermionic diode valve (vacuum tube). This used a hot cathode which permitted current to flow in a vacuum. This idea was quickly applied to X-ray tubes, and heated cathode X-ray tubes, called Coolidge tubes, replaced the troublesome cold cathode tubes by about 1920.
Two years later, physicist Charles Barkla discovered that X-rays could be scattered by gases, and that each element had a characteristic X-ray. He won the 1917 Nobel Prize in Physics for this discovery. Max von Laue, Paul Knipping and Walter Friedrich observed for the first time the diffraction of X-rays by crystals in 1912. This discovery, along with the early works of Paul Peter Ewald,William Henry Bragg and William Lawrence Bragg gave birth to the field of X-raycrystallography. The Coolidge tube was invented the following year by William D. Coolidge which permitted continuous production of X-rays; this type of tube is still in use today.
The use of X-rays for medical purposes (to develop into the field ofradiation therapy) was pioneered by Major John Hall-Edwards inBirmingham, England. In 1908, he had to have his left arm amputated owing to the spread of X-ray dermatitis.[51] The X-ray microscopewas invented in the 1950s.
The Chandra X-ray Observatory, launched on July 23, 1999, has been allowing the exploration of the very violent processes in the universe which produce X-rays. Unlike visible light, which is a relatively stable view of the universe, the X-ray universe is unstable, it features stars being torn apart by black holes, galactic collisions, and novas, neutron stars that build up layers of plasma that then explode into space.
An X-ray laser device was proposed as part of the Reagan Administration'sStrategic Defense Initiative in the 1980s, but the first and only test of the device (a sort of laser "blaster", or death ray, powered by a thermonuclear explosion) gave inconclusive results. For technical and political reasons, the overall project (including the X-ray laser) was de-funded (though was later revived by the secondBush Administration as National Missile Defense using different technologies).
[edit]See also
- Backscatter X-ray
- Fluoroscopy
- Geiger counter
- High energy X-rays
- N-ray
- Neutron radiation
- Radiography
- Radiologic technologist
- Radiology
- Resonant inelastic X-ray scattering (RIXS)
- Small angle X-ray scattering (SAXS)
- X-ray absorption spectroscopy
- X-ray astronomy
- X-ray crystallography
- X-Ray filters
- X-ray generation
- X-ray machine
- X-ray marker
- X-ray microscope
- X-ray nanoprobe
- X-ray optics
- X-ray vision
- X-ray welding
[edit]Notes
- ^ Novelline, Robert. Squire's Fundamentals of Radiology. Harvard University Press. 5th edition. 1997. ISBN 0674833392.
- ^ a b Dendy, P. P.; B. Heaton (1999). Physics for Diagnostic Radiology. USA: CRC Press. p. 12. ISBN 0750305916.
- ^ Charles Hodgman, Ed. (1961). CRC Handbook of Chemistry and Physics, 44th Ed.. USA: Chemical Rubber Co.. p. 2850.
- ^ Feynman, Richard; Robert Leighton, Matthew Sands (1963). The Feynman Lectures on Physics, Vol.1. USA: Addison-Wesley. pp. 2–5. ISBN 0201021161.
- ^ L'Annunziata, Michael; Mohammad Baradei (2003). Handbook of Radioactivity Analysis. Academic Press. p. 58. ISBN 0124366031.
- ^ Grupen, Claus; G. Cowan, S. D. Eidelman, T. Stroh (2005). Astroparticle Physics. Springer. p. 109. ISBN 3540253122.
- ^ US National Research Council (2006). Health Risks from Low Levels of Ionizing Radiation, BEIR 7 phase 2. National Academies Press. pp. 5, fig.PS–2. ISBN 030909156X., data credited to NCRP (US National Committee on Radiation Protection) 1987
- ^ http://www.doctorspiller.com/Dental%20_X-Rays.htm andhttp://www.dentalgentlecare.com/x-ray_safety.htm
- ^ http://hss.energy.gov/NuclearSafety/NSEA/fire/trainingdocs/radem3.pdf
- ^ http://www.hawkhill.com/114s.html
- ^ http://www.solarstorms.org/SWChapter8.html andhttp://www.powerattunements.com/x-ray.html
- ^ David R. Lide, ed (1994). CRC Handbook of Chemistry and Physics 75th edition. CRC Press. pp. 10–227. ISBN 0-8493-0475-X.
- ^ Kevles, Bettyann Holtzmann (1996). Naked to the Bone Medical Imaging in the Twentieth Century. Camden, NJ: Rutgers University Press. pp. 19–22.ISBN 0813523583.
- ^ Sample, Sharron (2007-03-27). "X-Rays". The Electromagnetic Spectrum.NASA. Retrieved 2007-12-03.
- ^ Whaites, Eric; Roderick Cawson (2002). Essentials of Dental Radiography and Radiology. Elsevier Health Sciences. pp. 15–20. ISBN 044307027X.
- ^ Bushburg, Jerrold; Anthony Seibert, Edwin Leidholdt, John Boone (2002).The Essential Physics of Medical Imaging. USA: Lippincott Williams & Wilkins. p. 116. ISBN 0683301187.
- ^ Emilio, Burattini; Antonella Ballerna (1994). "Preface". Biomedical Applications of Synchrotron Radiation: Proceedings of the 128th Course at the International School of Physics -Enrico Fermi- 12–22 July 1994, Varenna, Italy. IOS Press. pp. xv. ISBN 9051992483. Retrieved 2008-11-11.
- ^ Martin, Dylan (2005). "X-Ray Detection". University of Arizona Optical Sciences Center. Retrieved 2008-05-19.
- ^ Frame, Paul. "Wilhelm Röntgen and the Invisible Light". Tales from the Atomic Age. Oak Ridge Associated Universities. Retrieved 2008-05-19.
- ^ Eæements of Modern X-Ray Physics. John Wiley & Sons Ltd,. 2001. pp. 40–41. ISBN 0-471-49858-0.
- ^ a b Spiegel, Peter K (1995). "The first clinical X-ray made in America—100 years". American Journal of Roentgenology (Leesburg, VA: American Roentgen Ray Society) 164 (1): 241–243. ISSN: 1546-3141. PMID 7998549.
- ^ Herman, Gabor T. (2009). Fundamentals of Computerized Tomography: Image Reconstruction from Projections (2nd ed.). Springer. ISBN 978-1-85233-617-2
- ^ 11th Report on Carcinogens
- ^ Upton AC (2003).The state of the art in the 1990s: NCRP report No. 136 on the scientific bases for linearity in the dose-response relationship for ionizing radiation. Health Physics 85:15-22
- ^ United Nations Scientific Committee on the Effects of Atomic Radiation. New York. United Nations, 2000
- ^ Berrington de Gonzalez A and Darby S (2004). Risk of cancer from diagnostic X-rays: estimates for the UK and 14 other countries. Lancet 363: 345-351
- ^ a b Brenner DJ and Hall EJ (2007). Computed tomography- an increasing source of radiation exposure. New England Journal of Medicine 357: 2277-2284
- ^ a b [1]|Radiological Society of North America and American College of Radiology
- ^ [2]|National Cancer Institute: Surveillance Epidemiology and End Results (SEER) data
- ^ Xiao-Ou, Shu; et al (December 1994). "Association of paternal diagnostic X-ray exposure with risk of infant leukemia". Cancer Epidemiology, Biomarkers & Prevention (American Association for Cancer Research) 3 (8): 645. ISSN 1538-7755. PMID 7881337.
- ^ Stewart, Alice M; J.W. Webb; B.D. Giles; D. Hewitt, 1956. "Preliminary Communication: Malignant Disease in Childhood and Diagnostic Irradiation In-Utero," Lancet, 1956, 2: 447.
- ^ "Pregnant Women and Radiation Exposure". eMedicine Live online medical consultation. Medscape. 28 December 2008. Retrieved 2009-01-16.
- ^ Donnelly CF (2005). Reducing radiation dose associated with pediatric CT by decreasing unnecessary examinations. American Journal Roentgenology32: 242-244
- ^ Alchemy Art Lead Products – Lead Shielding Sheet Lead For Shielding Applications, retrieved 2008-12-07
- ^ Kasai, Nobutami; Masao Kakudo (2005). X-ray diffraction by macromolecules. Tokyo: Kodansha. pp. 291–2. ISBN 3540253173.
- ^ The history, development, and impact of computed imaging in neurological diagnosis and neurosurgery: CT, MRI, DTI: Nature Precedings DOI: 10.1038/npre.2009.3267.5.
- ^ a b c Gaida, Roman; et al. (1997). "Ukrainian Physicist Contributes to the Discovery of X-Rays". Mayo Foundation for Medical Education and Research. Retrieved 2008-04-06.
- ^ Morton, William James, and Edwin W. Hammer, American Technical Book Co., 1896. Page 68.
- ^ U.S. Patent 514,170, Incandescent Electric Light, and U.S. Patent 454,622, System of Electric Lighting.
- ^ Cheney, Margaret, "Tesla: Man Out of Time ". Simon and Schuster, 2001. Page 77.
- ^ Thomas Commerford Martin (ed.), "The Inventions, Researches and Writings of Nikola Tesla". Page 252 "When it forms a drop, it will emit visible and invisible waves. [...]". (ed., this material originally appeared in an article by Nikola Tesla in The Electrical Engineer of 1894.)
- ^ Nikola Tesla, "The stream of Lenard and Roentgen and novel apparatus for their production", Apr. 6, 1897.
- ^ Cheney, Margaret, Robert Uth, and Jim Glenn, "Tesla, master of lightning". Barnes & Noble Publishing, 1999. Page 76. ISBN 0760710058
- ^ Wyman, Thomas (Spring 2005). "Fernando Sanford and the Discovery of X-rays". "Imprint", from the Associates of the Stanford University Libraries: 5–15.
- ^ Thomson, Joseph J. (1903). The Discharge of Electricity through Gasses. USA: Charles Scribner's Sons. pp. 182–186.
- ^ Thomson, 1903, p.185
- ^ Wiedmann's Annalen, Vol. XLVIII
- ^ Stanton, Arthur (1896-01-23). "Wilhelm Conrad Röntgen On a New Kind of Rays: translation of a paper read before the Würzburg Physical and Medical Society, 1895" (Subscription-only access – Scholar search). Nature 53(1369): 274–6. doi:10.1038/053274b0 see also pp. 268 and 276 of the same issue.
- ^ Peters, Peter (1995). "W. C. Roentgen and the discovery of x-rays". Ch.1 Textbook of Radiology. Medcyclopedia.com, GE Healthcare. Retrieved 2008-05-05.
- ^ National Library of Medicine. "Could X-rays Have Saved President William McKinley?" Visible Proofs: Forensic Views of the Body.http://www.nlm.nih.gov/visibleproofs/galleries/cases/mckinley.html
- ^ [3]
[edit]References
- NASA Goddard Space Flight centre introduction to X-rays.
[edit]External links
| Wikimedia Commons has media related to: X-ray |
| Look up x-ray in Wiktionary, the free dictionary. |
- Example Radiograph: Fractured Humerus
- A Photograph of an X-ray Machine
- X-ray Safety
- An X-ray tube demonstration (Animation)
- 1896 Article: "On a New Kind of Rays"
- "Digital X-Ray Technologies Project"
- A video of a medical X-ray procedure example
- What is Radiology? a simple tutorial
- 50,000 X-ray, MRI, and CT pictures MedPix medical image database
- Index of Early Bremsstrahlung Articles
- Extraordinary X-Rays - slideshow by Life magazine









Tidak ada komentar:
Posting Komentar